Reshaping Dental Care with Synthetic Intelligence

Artificial intelligence has transformed industries worldwide in recent years, and dentistry is no exception. The concept of machines being able to carry out human jobs is known as “artificial intelligence” (AI).1 By mimicking human intelligence, AI enhances rather than replaces human expertise.2 AI’s integration into dental practices has revolutionized patient care, from appointment scheduling to follow-up procedures, by improving disease detection, treatment methods, and access to care.3 Dental practices reliant on digital technologies like computers and X-ray machines, benefit significantly from AI, enhancing efficiency and patient outcomes. Ongoing research continues to advance AI’s capabilities in dentistry. Machine learning (ML) is a type of AI that allows computer systems to learn from past experiences or data without being explicitly programmed. One specific type of ML technique, Artificial Neural Networks (ANNs), is designed to mimic brain function, enabling computers to learn autonomously without human intervention. Deep Learning (DL) is a subgroup of ANNs that involves multi-layered networks, allowing computers to process complex information. DL techniques, particularly convolutional neural networks (CNNs), are well-suited for tasks like recognizing and analyzing dental images.1 This article aims to explore current AI applications in various dental specialties, emphasize collaborative partnerships with human expertise, envision future directions, demonstrate efficiency gains, and offer a detailed overview of AI’s role in enhancing patient outcomes, serving as a valuable resource for dental practitioners and researchers.
General Dentistry (Fig. 1)
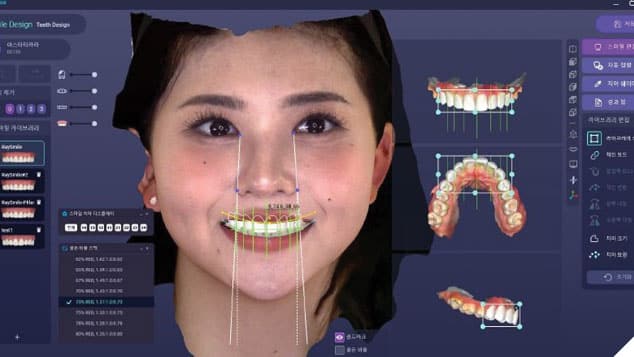
AI plays a crucial role in modern dental practices by providing easy access to electronic health records (EHRs) and assisting in the prompt detection of abnormalities. It enhances efficiency and precision in dental care through AI-driven virtual dental assistants, which streamline administrative tasks and aid in diagnosis and treatment planning. AI also helps shorten chairside time, improve infection control, and ensure high-quality treatment. Innovations such as medical scribe websites further streamline documentation processes by automatically transcribing patient conversations into SOAP notes.4
Prosthodontics (Fig. 2)
AI revolutionizes prosthodontics by optimizing personalized care through data management. Convolutional Neural Networks (CNNs) predict and categorize dental arches, guiding tailored designs for partial dentures.5 AI aids in creating crown occlusal surfaces, complete denture designs, and optimized implantology profiles, while automating jaw connection registration for treatment simulations. Teamed with CAD/CAM technology, AI enhances prostheses aesthetics and reduces failure rates.6 AI-driven tools improve diagnostics, crown and denture precision, and prolong prosthetic longevity and functionality.7 Intraoral scanners, powered by AI, ensure accurate digital impressions, expediting clinical and lab workflows.8 This integration accelerates design and manufacturing, adhering to patient-centric care principles.9
Endodontics (Fig. 3)
AI revolutionizes endodontics, offering precise diagnostics and treatment planning with remarkable accuracy.10 ML algorithms optimize root canal treatment, predicting personalized instrumentation and irrigation protocols, leading to successful outcomes and fewer complications.11 Innovations like Navident offer user-friendly, precise solutions for virtual planning in endodontics, enhancing procedural precision, while AI’s clinical applications in the field include detecting root fractures, periapical pathologies, and assessing root morphology to improve procedural outcomes, with guided endodontic platforms further enhancing navigation and treatment planning to ensure ideal results.12-14
Periodontology (Fig. 4)
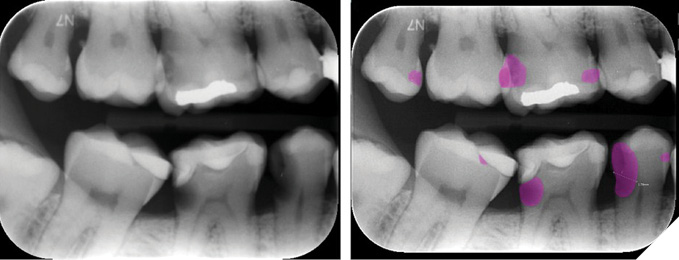
AI enhances periodontics by improving image analysis and diagnostic accuracy, with deep learning interpreting alveolar bone and assessing disease severity. ANNs classify periodontitis types, while machine learning ML corrects imaging errors and detects caries. Mask R-CNN is crucial in CBCT scans for precise dental implant planning and identifying anatomical structures, and for calculating radiographic bone loss rates to optimize implant assessments.15
Orthodontics (Fig. 5)
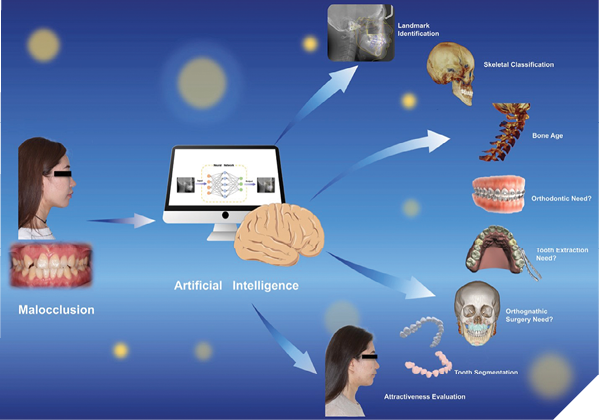
AI plays a vital role in orthodontic treatment by identifying anatomic landmarks across radiographic modalities, aiding in precise treatment planning and optimization.16 DL evaluates maxillary asymmetry and forecasts orthodontic needs using radiographic scans, analyzes 3D dental models, and optimizes treatment duration, while the YOLO method diagnoses malocclusion with accuracy and precision.17 AI-driven orthodontic software generates personalized treatment plans, particularly evident in clear aligner design, ensuring optimal alignment and treatment efficiency.18
Pediatric Dentistry (Fig. 6)
The AI system demonstrated a performance that was clinically acceptable for identifying dental plaque on primary teeth, comparable to that of a skilled pediatric dentist.19 In the field of pediatric dentistry, AI holds considerable promise for transforming behavioral practices; tools such as 4D goggles, films, animations, and virtual reality games have proven to be effective behavioral modification aids for young patients.20
Dental Anesthesiology (Fig. 7)
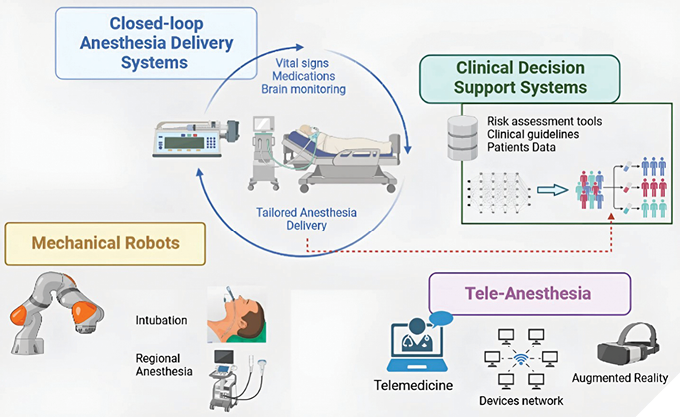
Computer-assisted systems in dental anesthesia help regulate injection pressure and strength for reduced discomfort and improved patient comfort during local anesthetic administration. A scoping review outlined six main clinical applications of AI in dental anesthesiology, such as monitoring and controlling anesthesia, predicting risks, guiding ultrasonography, pain management, and improving operating room logistics.21 However, research on AI’s impact on clinical treatment in dental anesthesia is limited, with few studies examining its integration into regular clinical workflows.22
Oral Surgery (Fig. 8)
AI shows promise in oral maxillofacial surgery, aiding in robotic cranial surgeries with positive outcomes. AI tools utilizing cephalometric measurements and imaging scans support treatment decision-making during orthodontic surgeries for patients with dentofacial deformities, although standardizing these AI assessments remains challenging.23 AI predicts third molar eruption potential from panoramic radiographs, aiding tooth extraction decisions,24 while integrating VR and IoT enhances surgical planning with 3D visualizations and improved device connectivity, and VR additionally improves patient education and decision-making participation.25
Oral Radiology (Fig. 9)
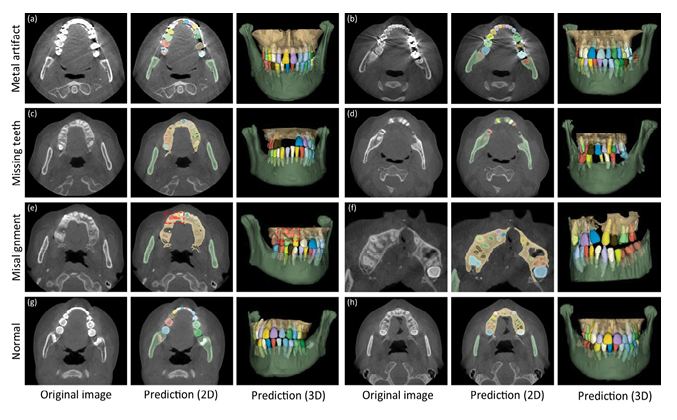
AI effectively identifies impacted supernumerary teeth on panoramic radiographs and aids in detecting various dental conditions, including cysts, tumors, and periodontal disease, through DL techniques.26, 27 DL algorithms integrated into CAD systems assist in diagnosing periodontal bone loss and osteoporosis based on panoramic photographs, revolutionizing clinical and X-ray diagnoses. CBCT provides detailed three-dimensional images, aiding in diagnosing impacted teeth, temporomandibular joint disorders, and jawbone pathologies with superior accuracy.28
Oral Medicine (Fig. 10)
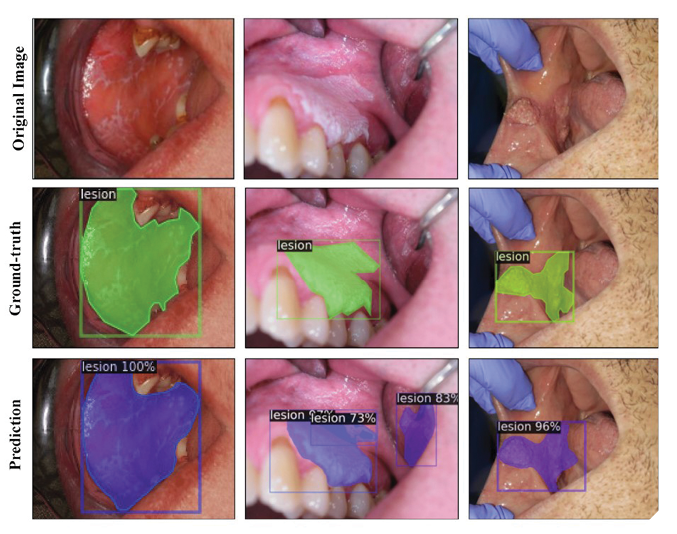
AI-based models, particularly those using Mask R-CNN ResNeXt-FPN, enhance oral lesion classification from clinical images, improving early detection and diagnostic accuracy of premalignant lesions and cancer.29 Utilizing vast biomarker data, AI streamlines the detection and classification of dental conditions, including root caries, BRONJ, and facial defects, in radiographs and aids in the prompt diagnosis and treatment of periodontal disease, sinusitis, arthritic changes in TMJ disorders, and Oral Squamous Cell Carcinoma.30
Oral Pathology (Fig. 11)
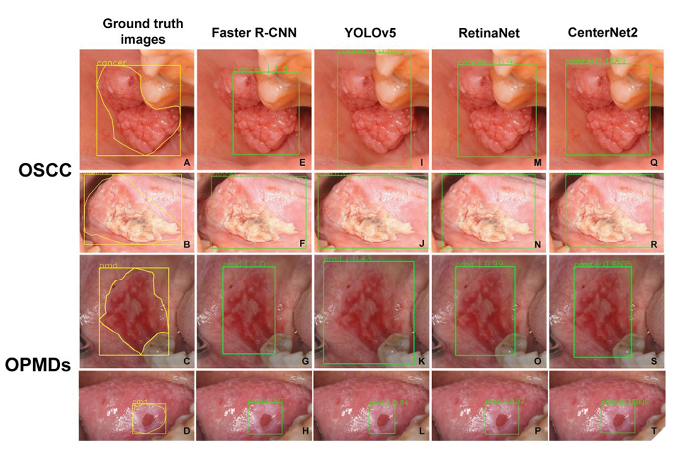
Limited research exists on AI’s role in diagnosing potential cancerous or premalignant head and neck lesions, yet AI and ML methods show effectiveness akin to traditional histopathology, offering faster, unbiased, and reproducible evaluations.31 AI has shown promise in early oral cancer detection using laser-induced autofluorescence spectra and artificial neural networks.32 CNN-based models like DenseNet-169 and ResNet-101 matched or surpassed expert-level performance in classifying oral cancers and oral potentially malignant disorders (OPMDs), offering a promising diagnostic tool for enhancing early detection in screening programs.33
Orofacial Pain (Fig. 12)
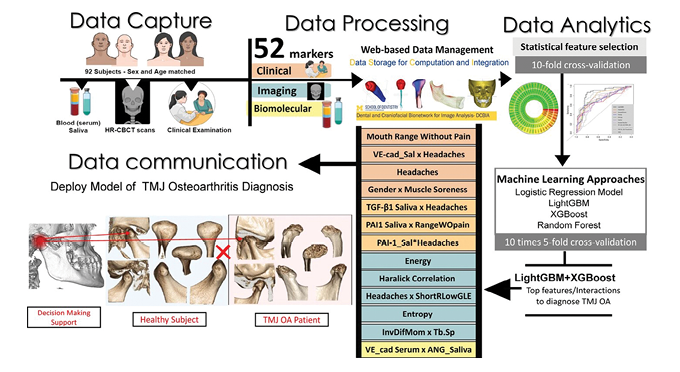
AI assists Orofacial Pain Specialists by analyzing patient-reported data, aiding in diagnosing various orofacial pain conditions and developing tailored treatment strategies.34 It is pivotal in the multifaceted diagnosis and treatment of Temporomandibular Disorders (TMD), including the design of orthotic devices and the classification of sleep disorders such as obstructive sleep apnea (OSA).35, 36 AI-driven tools, including ANN and CNN, support precise diagnosis and development of targeted treatments, significantly improving clinical decision-making and treatment accuracy.37, 38
Dental Public Health (Fig. 13)
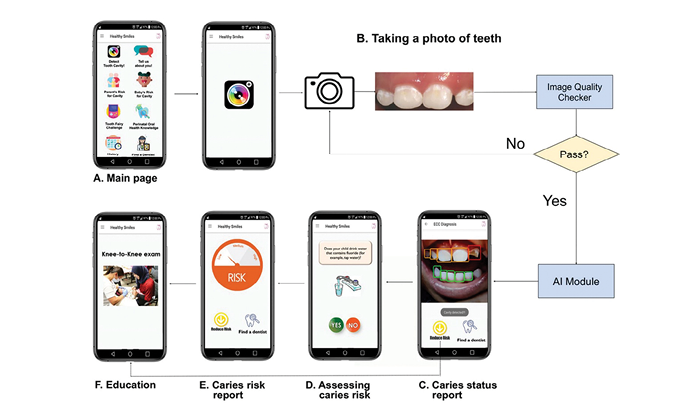
AI is pivotal in preventive dentistry, aiding early interventions and ongoing patient data monitoring. It optimizes preventive treatment planning like resin restoration, enhancing long-term oral health. Mobile health apps in dental public health, empowered by AI-driven data analysis, elevate patient engagement and education. AI’s predictive analytics leverage extensive datasets to forecast dental health trends and identify at-risk groups, vital for crafting targeted preventive programs that cut health costs and boost public outcomes.39 While unsupervised machine learning progresses, primary care health informatics is crucial for safe AI integration in dental practices. AI’s evolution could revolutionize routine screening and specialized diagnostics in medicine and public health in underserved areas.40, 41
Practice Management (Fig. 14)
AI streamlines practice management by optimizing appointment scheduling, enhancing resource efficiency, reducing no-shows, and enhancing patient experiences. Tools like chatbots and virtual assistants provide personalized interactions and reminders. AI also automates HIPAA-compliant consent forms, extracts data using NLP, manages insurance data, streamlines claims processing, and facilitates secure payment processing, simplifying administrative tasks and improving financial operations.42
Future Directions (Fig. 15)

The paper envisions AI’s potential applications in dentistry, including advancements in lesion detection, early prediction, enhanced image quality, and reduced radiation exposure, promising to enhance the overall patient experience in dental clinics.
Conclusion
Artificial intelligence profoundly transforms dentistry, improving diagnostic accuracy, treatment planning, and patient care. The collaborative partnership between AI and human expertise augments dental professionals’ capabilities, driving efficiency, innovation, and improved outcomes in oral healthcare. Envisioning future advancements like improved lesion detection and image quality underscores AI’s ongoing evolution in reshaping modern dentistry for the better.
References
- Schwendicke F, Samek W, Krois J. Artificial Intelligence in Dentistry: Chances and Challenges. J Dent Res 2020;99(7):769-74.
- 2Dindorf C, Bartaguiz E, Gassmann F, Fröhlich M. Conceptual Structure and Current Trends in Artificial Intelligence, Machine Learning, and Deep Learning Research in Sports: A Bibliometric Review. Int J Environ Res Public Health 2022;20(1).
- Bohr A MK. The rise of artificial intelligence in healthcare applications. Artificial Intelligence in Healthcare 2020;2020:25–60.
- van Buchem MM, Boosman H, Bauer MP, et al. The digital scribe in clinical practice: a scoping review and research agenda. NPJ Digit Med 2021;4(1):57.
- Revilla-León M, Gómez-Polo M, Vyas S, et al. Artificial intelligence models for tooth-supported fixed and removable prosthodontics: A systematic review. J Prosthet Dent 2023;129(2):276-92.
- Singi SR, Sathe S, Reche AR, Sibal A, Mantri N. Extended Arm of Precision in Prosthodontics: Artificial Intelligence. Cureus 2022;14(11):e30962.
- Grischke J, Johannsmeier L, Eich L, Griga L, Haddadin S. Dentronics: Towards robotics and artificial intelligence in dentistry. Dent Mater 2020;36(6):765-78.
- Christopoulou I, Kaklamanos EG, Makrygiannakis MA, et al. Intraoral Scanners in Orthodontics: A Critical Review. Int J Environ Res Public Health 2022;19(3).
- Chau RCW, Hsung RT, McGrath C, Pow EHN, Lam WYH. Accuracy of artificial intelligence-designed single-molar dental prostheses: A feasibility study. J Prosthet Dent 2023.
- Aminoshariae A, Kulild J, Nagendrababu V. Artificial Intelligence in Endodontics: Current Applications and Future Directions. J Endod 2021;47(9):1352-57.
- Lai G, Dunlap C, Gluskin A, Nehme WB, Azim AA. Artificial Intelligence in Endodontics. Journal of the California Dental Association 2023;51(1):2199933.
- Connert T, Leontiev W, Dagassan-Berndt D, et al. Real-Time Guided Endodontics with a Miniaturized Dynamic Navigation System Versus Conventional Freehand Endodontic Access Cavity Preparation: Substance Loss and Procedure Time. J Endod 2021;47(10):1651-56.
- Dianat O, Gupta S, Price JB, Mostoufi B. Guided Endodontic Access in a Maxillary Molar Using a Dynamic Navigation System. J Endod 2021;47(4):658-62.
- Gambarini G, Galli M, Morese A, et al. Precision of Dynamic Navigation to Perform Endodontic Ultraconservative Access Cavities: A Preliminary In Vitro Analysis. J Endod 2020;46(9):1286-90.
- Chang HJ, Lee SJ, Yong TH, et al. Deep Learning Hybrid Method to Automatically Diagnose Periodontal Bone Loss and Stage Periodontitis. Sci Rep 2020;10(1):7531.
- Kim H, Shim E, Park J, et al. Web-based fully automated cephalometric analysis by deep learning. Comput Methods Programs Biomed 2020;194:105513.
- Liu J, Chen Y, Li S, Zhao Z, Wu Z. Machine learning in orthodontics: Challenges and perspectives. Adv Clin Exp Med 2021;30(10):1065-74.
- Castroflorio T, Sedran A, Parrini S, et al. Predictability of orthodontic tooth movement with aligners: effect of treatment design. Prog Orthod 2023;24(1):2.
- You W, Hao A, Li S, Wang Y, Xia B. Deep learning-based dental plaque detection on primary teeth: a comparison with clinical assessments. BMC Oral Health 2020;20(1):141.
- Baliga SM. Artificial intelligence – The next frontier in pediatric dentistry. Journal of Indian Society of Pedodontics and Preventive Dentistry 2019;37(4):315.
- Hashimoto DA, Witkowski E, Gao L, Meireles O, Rosman G. Artificial Intelligence in Anesthesiology: Current Techniques, Clinical Applications, and Limitations. Anesthesiology 2020;132(2):379-94.
- Cascella M, Tracey M, Petrucci E, Bignami EG. Exploring Artificial Intelligence in Anesthesia: A Primer on Ethics, and Clinical Applications: Preprints.org; 2023.
- Nogueira-Reis F, Morgan N, Nomidis S, et al. Three-dimensional maxillary virtual patient creation by convolutional neural network-based segmentation on cone-beam computed tomography images. Clin Oral Investig 2023;27(3):1133-41.
- Vranckx M, Van Gerven A, Willems H, et al. Artificial Intelligence (AI)-Driven Molar Angulation Measurements to Predict Third Molar Eruption on Panoramic Radiographs. Int J Environ Res Public Health 2020;17(10).
- Javaid M, Haleem A, Pratap Singh R, Suman R. Pedagogy and innovative care tenets in COVID-19 pandemic: An enhancive way through Dentistry 4.0. Sens Int 2021;2:100118.
- Lee JH, Kim DH, Jeong SN, Choi SH. Detection and diagnosis of dental caries using a deep learning-based convolutional neural network algorithm. J Dent 2018;77:106-11.
- Orhan K, Bayrakdar IS, Ezhov M, Kravtsov A, Özyürek T. Evaluation of artificial intelligence for detecting periapical pathosis on cone-beam computed tomography scans. Int Endod J 2020;53(5):680-89.
- Cui Z, Fang Y, Mei L, et al. A fully automatic AI system for tooth and alveolar bone segmentation from cone-beam CT images. Nat Commun 2022;13(1):2096.
- Tanriver G, Soluk Tekkesin M, Ergen O. Automated Detection and Classification of Oral Lesions Using Deep Learning to Detect Oral Potentially Malignant Disorders. Cancers (Basel) 2021;13(11).
- Ilhan B, Lin K, Guneri P, Wilder-Smith P. Improving Oral Cancer Outcomes with Imaging and Artificial Intelligence. J Dent Res 2020;99(3):241-48.
- Mahmood H, Shaban M, Indave BI, et al. Use of artificial intelligence in diagnosis of head and neck precancerous and cancerous lesions: A systematic review. Oral Oncol 2020;110:104885.
- Nayak GS, Kamath S, Pai KM, et al. Principal component analysis and artificial neural network analysis of oral tissue fluorescence spectra: classification of normal premalignant and malignant pathological conditions. Biopolymers 2006;82(2):152-66.
- Warin K, Limprasert W, Suebnukarn S, et al. AI-based analysis of oral lesions using novel deep convolutional neural networks for early detection of oral cancer. PLoS One 2022;17(8):e0273508.
- Naseri H, Kafi K, Skamene S, et al. Development of a generalizable natural language processing pipeline to extract physician-reported pain from clinical reports: Generated using publicly-available datasets and tested on institutional clinical reports for cancer patients with bone metastases. J Biomed Inform 2021;120:103864.
- Bazoukis G, Bollepalli SC, Chung CT, et al. Application of artificial intelligence in the diagnosis of sleep apnea. J Clin Sleep Med 2023;19(7):1337-63.
- Lee KS, Kwak HJ, Oh JM, et al. Automated Detection of TMJ Osteoarthritis Based on Artificial Intelligence. J Dent Res 2020;99(12):1363-67.
- Kumar Y, Koul A, Singla R, Ijaz MF. Artificial intelligence in disease diagnosis: a systematic literature review, synthesizing framework and future research agenda. J Ambient Intell Humaniz Comput 2023;14(7):8459-86.
- Ozsari S, Güzel MS, Yılmaz D, Kamburoğlu K. A Comprehensive Review of Artificial Intelligence Based Algorithms Regarding Temporomandibular Joint Related Diseases. Diagnostics (Basel) 2023;13(16).
- Al-Jallad N, Ly-Mapes O, Hao P, et al. Artificial intelligence-powered smartphone application, AICaries, improves at-home dental caries screening in children: Moderated and unmoderated usability test. PLOS Digit Health 2022;1(6).
- Beam AL, Kohane IS. Translating Artificial Intelligence Into Clinical Care. Jama 2016;316(22):2368-69.
- Benke K, Benke G. Artificial Intelligence and Big Data in Public Health. Int J Environ Res Public Health 2018;15(12).
- Pethani F, Dunn AG. Natural language processing for clinical notes in dentistry: A systematic review. J Biomed Inform 2023;138:104282.
About the Author

Dr. Amey G. Patil, a cosmetic dentist and board-certified orofacial pain specialist, is Assistant Professor and Director, General Dental Concepts at the Temporomandibular Disorders and Orofacial Pain Center, Diagnostic Sciences, at Rutgers. He is a Diplomate of the American Board of Orofacial Pain (DABOP) and Fellow, International College of Dentists (FICD), American College of Dentists (FACD), Pierre Fauchard Academy (FPFA), International Academy for Dental-Facial Esthetics (FIADFE), and American Academy of Orofacial Pain (FAAOP). The inventor of the pico-hydroelectric toothbrush, Dr. Patil speaks internationally on AI, esthetics and orofacial pain.




